The fluoropyrimidine 5-fluorouracil (5-FU) and its prodrug capecitabine are cytotoxic agents that have been widely used in the treatment of solid tumors. In the United States alone, an estimated 275,000 patients with cancer receive 5-FU each year.1 Despite its lifesaving/life-prolonging potential, 5-FU causes severe early-onset toxicity in up to one-fourth of patients, and more than 1300 die each year as a result of this toxicity.1,2 Until recently, treatment for 5-FU or capecitabine overexposure was limited to supportive care and symptomatic treatment, which resulted in unacceptably high mortality.
In 2015, uridine triacetate was approved by the US Food and Drug Administration (FDA) for adult and pediatric patients who exhibit early-onset severe or life-threatening 5-FU/capecitabine toxicities or who present with an overdose.3 Approval was based on data from 2 single-arm, open-label, expanded-access trials of 135 patients who received uridine triacetate for 5-FU or capecitabine overdose, or who exhibited severe or life-threatening toxicities within 96 hours of the end of treatment with these fluoropyrimidines.3 Of these patients, 96% had survived at the 30-day follow-up cutoff, with minor adverse reactions that included vomiting, nausea, and diarrhea.3
This article provides an overview of 5-FU and capecitabine, including the common causes for their early-onset severe toxicity and overdose, as well as final overall safety and efficacy data on uridine triacetate in 2 international, compassionate-use, open-label clinical studies. These data support the use of uridine triacetate as a lifesaving antidote for patients with overexposure to 5-FU or capecitabine.
Overview of 5-FU and Capecitabine
5-FU is a synthetic pyrimidine analog that has been used to treat a variety of solid tumors since its clinical introduction in the late 1950s.4 With activity in treating cancers of the head and neck, breast, prostate, pancreas, liver, and genitourinary and gastrointestinal (GI) tracts, 5-FU has been commonly used as monotherapy and in combination with other chemotherapeutics and radiation.5,6 When delivered orally, 5-FU has variable absorption in the gut5 and is rapidly degraded by the liver7; therefore, it is limited to intravenous administration.
In 1998, the orally bioavailable 5-FU prodrug capecitabine, which is converted to 5-FU in 3 metabolic steps, was approved by the FDA for use in the United States.7,8 Because the final metabolic step in activating capecitabine to 5-FU requires thymidine phosphorylase, an enzyme commonly found at higher levels in tumor cells than in healthy cells, capecitabine is theoretically capable of enhanced targeting of cancerous tissue while reducing systemic toxicity.7 Nevertheless, the narrow therapeutic index of 5-FU and capecitabine results in early-onset severe or life-threatening toxicity in as many as 25% of patients receiving fluoropyrimidine-containing regimens and an estimated toxicity-related mortality rate of 0.5% to 1.0%.2,3,9
Early-Onset Toxicity and Overdose with 5-FU and Capecitabine
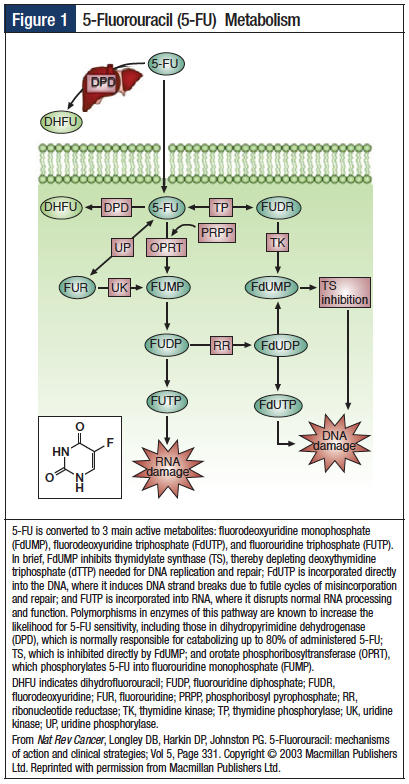
5-FU and capecitabine are inert antimetabolites that must be metabolized intracellularly into the active cytotoxic metabolites fluorodeoxyuridine monophosphate (FdUMP), fluorodeoxyuridine triphosphate (FdUTP), and fluorouridine triphosphate (FUTP) (Figure 1).10 Only approximately 1% to 3% of administered 5-FU and capecitabine is converted into these cytotoxic metabolites, with more than 80% of 5-FU being rapidly catabolized by dihydropyrimidine dehydrogenase (DPD) and subsequently eliminated.2,5,11 FdUMP, FdUTP, and FUTP induce cell death by inhibiting the synthesis of thymidine, which leads to defective DNA replication5; being misincorporated into DNA and inducing DNA strand breaks10; and being incorporated into RNA and disrupting normal RNA processing and function (ie, protein synthesis),12 respectively. Like other cytotoxic chemotherapies, the activity of fluoropyrimidine is not specific to cancer cells but also affects rapidly dividing healthy cells. For 5-FU, the most common dose-limiting toxicities are myelosuppression, mucositis, and diarrhea,13 whereas for capecitabine, the main toxicities are hand-foot syndrome, diarrhea, and stomatitis.9
5-FU is typically administered over several days at or near its maximum tolerated dose, leading to the potential for increased toxicity.14 This results in early-onset severe or life-threatening toxicity in as many as 25% of patients.2 For capecitabine, as many as 40% of patients experienced severe treatment-related toxicity in pivotal studies.15 Furthermore, toxicity-related dose reductions have been necessary in up to 49% of patients receiving 5-FU and up to 41% of patients receiving capecitabine.5 Patients who are sensitive to 5-FU and capecitabine and who receive standard doses of these drugs can have early-onset toxicities during or after their first course of treatment and can present as a massive overdose.16,17 Toxicity to 5-FU increases with a patient’s pharmacokinetic exposure (ie, area under the curve), which itself is a function of the medication’s dose, infusion rate, and the patient’s rate of clearance.16,18 Therefore, patient-related factors that modify 5-FU exposure, such as renal impairment, body surface area (BSA), age, and certain genetic variants, including polymorphisms of DPD, thymidylate synthase (TS), and orotate phosphoribosyltransferase (OPRT), have been associated with early-onset toxicity.12,15 Deficiency in DPD alone has been estimated to account for approximately 50% of all early-onset toxicities.15 However, screening of a patient’s DPD activity prior to initiation of 5-FU or capecitabine therapy is not routinely performed, and accurate prognostic tests for patients at high risk for early-onset toxicity have yet to be developed.3
Personalized dosing of 5-FU is challenging, with common BSA-based dosing algorithms leading to an estimated 40% to 60% of patients being underdosed and 10% to 20% of patients being overdosed.19 Fluoropyrimidine overdose, either by accident or suicidal intent, is a rare but serious event that can result in significant morbidity and mortality.3 In addition to poor dosing algorithms, reported causes of accidental overdose in the clinic have included infusion pump malfunctions,3,20 incorrect pump programming,3,21 use of an incorrect pump,21 and dosage miscalculations.21 For capecitabine, which is administered in tablet form and can be taken at home, overdose has occurred in attempted suicides as well as in accidental ingestion by children.16
Regardless of the mode of overexposure, the first signs of complications can occur within hours to days of dosing.22 Initial effects are typically GI in nature and include nausea, vomiting, diarrhea, ulceration, stomatitis, mucositis, and esophagopharyngitis.20,22 Cytopenia generally follows, with a delayed onset of 9 to 14 days after exposure.20 Cardiotoxicity, which usually appears 2 to 5 days after the initial exposure,22 is the most common cause of death, although the precise molecular mechanisms by which the heart is affected are not fully known.1,4 Neurotoxic complications, including hyperammonemia, acute encephalopathy, and cerebellar ataxia, may also occur.22
Treatment Options for 5-FU and Capecitabine Overexposure
Traditional treatment for overexposure to 5-FU and capecitabine was limited to supportive care, which commonly included the administration of colony-stimulating factors to overcome cytopenia and antibiotics to prevent infection/sepsis.20 Other symptomatic treatments included antiemetics, intravenous fluids, and intensive care.16 Unfortunately, the efficacy of the supportive care paradigm has generally been poor. In a case record review of 25 patients who experienced 5-FU overdoses and underwent supportive care, only 4 (16%) survived.16
In December 2015, the FDA approved the first therapy for the treatment of serious or life-threatening toxicities after 5-FU or capecitabine exposure.3 Uridine triacetate is indicated for the emergency treatment of adult and pediatric patients who have experienced a 5-FU or capecitabine overdose regardless of the presence of symptoms, or who exhibit early-onset, severe or life-threatening toxicity within 96 hours following the end of 5-FU or capecitabine administration.23
Uridine triacetate, an acetylated prodrug of uridine, is converted into uridine by nonspecific esterases in the blood.23 A further metabolic step converts this circulating uridine into uridine triphosphate that competes with FUTP for incorporation into RNA.3 Preventing the incorporation of FUTP into RNA mitigates the cell damage and cell death caused by 5-FU and capecitabine.3 Early clinical and animal studies have shown that uridine itself can prevent or reduce 5-FU–related toxicity and mortality.3 However, neither oral nor parenteral infusion of uridine is clinically feasible because of poor bioavailability and safety issues, respectively.16 Uridine triacetate, on the other hand, has 4- to 6-fold better oral bioavailability than uridine itself at equimolar doses and has been shown to be a safe and effective oral antidote to 5-FU overexposure in animals.16,24
Pivotal Clinical Trials of Uridine Triacetate
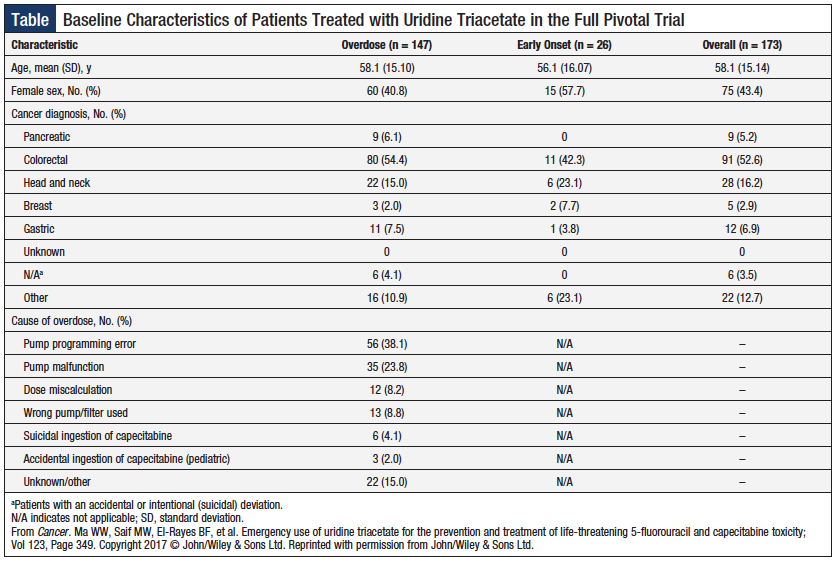
The final data from 2 open-label trials evaluating the overall safety and efficacy of uridine triacetate were recently published.16 These studies were conducted at sites in the United States, Europe, Canada, and Australia and included 173 adult and pediatric patients, all of whom were at increased risk for 5-FU toxicity caused by overdose, had demonstrated a rapid onset of severe toxicity, or were suspected to have increased susceptibility to 5-FU (eg, a patient known to be DPD-deficient). Full baseline characteristics of these patients can be found in the Table.16 All patients received uridine triacetate 10 g orally every 6 hours, for a total of 20 doses, with treatment starting as soon as possible after receiving 5-FU or capecitabine and after recognizing the need for antidotal treatment. Because withholding treatment (ie, using a placebo) would have been unethical, a historic control cohort comprising 5-FU overdose cases collected from the published literature, FDA, and the Institute for Safe Medication Practices was used as a comparator. The overall primary end point of these studies was survival or resumption of chemotherapy during the 30-day monitoring period. Adverse events were also monitored during the same 30-day period.
Of the 173 patients in these studies, 26 presented with early-onset severe toxicity, which was defined as those toxicities that occurred during or within 96 hours of 5-FU administration or during a standard 14-day course of capecitabine. Observed toxicities included severe cytotoxic mucosal and/or hematologic toxicities as well as acute encephalopathy and/or cardiomyopathy. The majority of these early-onset toxicities occurred after a patient’s first exposure, suggesting that these patients were unusually susceptible to fluoropyrimidines. For 18 early-onset patients, treatment with uridine triacetate was initiated within 96 hours of the termination of 5-FU or capecitabine. Strikingly, all 18 (100%) of these patients survived to the predetermined 30-day study end point. Of the 8 early-onset patients who received uridine triacetate after 96 hours, only 3 (38%) survived; the 5 deaths were attributed to sequelae of 5-FU toxicities, including acute respiratory distress syndrome (n = 1), multisystem organ failure secondary to sepsis (n = 1), and septic shock (n = 3).
The remaining 147 patients in this study were patients who received overdoses of 5-FU or capecitabine, with the most common causes being infusion pump programming errors (n = 56; 38.1%) and pump malfunctions (n = 35; 23.8%) with 5-FU, and intentional overdoses (n = 6) and accidental pediatric overdoses (n = 3) with capecitabine. All overdose patients had received 1.9 to 576 times the planned infusion rate of 5-FU or doses up to 10 times higher than intended. Of the 142 evaluable patients receiving uridine triacetate (5 were lost to follow-up), 137 (96%) survived to the 30-day end of follow-up versus 4 of 25 patients (16%) who received only supportive care in the historic control group. Notably, of the 141 overdose patients with cancer who were eligible to resume chemotherapy, 53 (38%) did so within the 30-day observation period, with most resuming treatment in <3 weeks (mean time to resumption of therapy, 19.6 days).
Uridine triacetate was well tolerated in the pivotal trial.16 Adverse reactions reported at a frequency of ≥2% were vomiting (n = 14; 8.1%), nausea (n = 8; 4.6%), and diarrhea (n = 6; 3.5%). One patient with head and neck cancer who had a previous history of serious nausea and vomiting reported grade 3 nausea and vomiting while receiving uridine triacetate. It should be noted that the adverse events reported during the use of uridine triacetate were consistent with those generally observed with chemotherapy.
Discussion
5-FU and capecitabine are mainstays of cancer treatment, even though their narrow therapeutic indices pose the threat of inadvertent overdose and severe early-onset toxicity. Although the true number of overdoses is unknown, an estimated 10% to 20% of patients receiving 5-FU are overdosed using BSA-based dosing algorithms,19 a figure that does not account for clinical mishaps such as infusion pump programming errors and pump malfunctions, or accidental ingestion of capecitabine. It is therefore likely that a substantial number of 5-FU and capecitabine overdoses go unreported.
Until recently, treatment of patients with severe early-onset toxicity or overdose with 5-FU or capecitabine was limited to supportive therapy, which had poor historic efficacy in preventing patient mortality. In a historic control cohort of 25 patients with 5-FU overdoses, only 16% receiving supportive therapy survived.16 Given that more than 1300 patients in the United States die each year from 5-FU–related toxicity,1 and that early-onset, severe or life-threatening toxicity may affect as many as 25% of treated patients,2 an effective antidote to 5-FU or capecitabine overexposure has been clearly lacking.
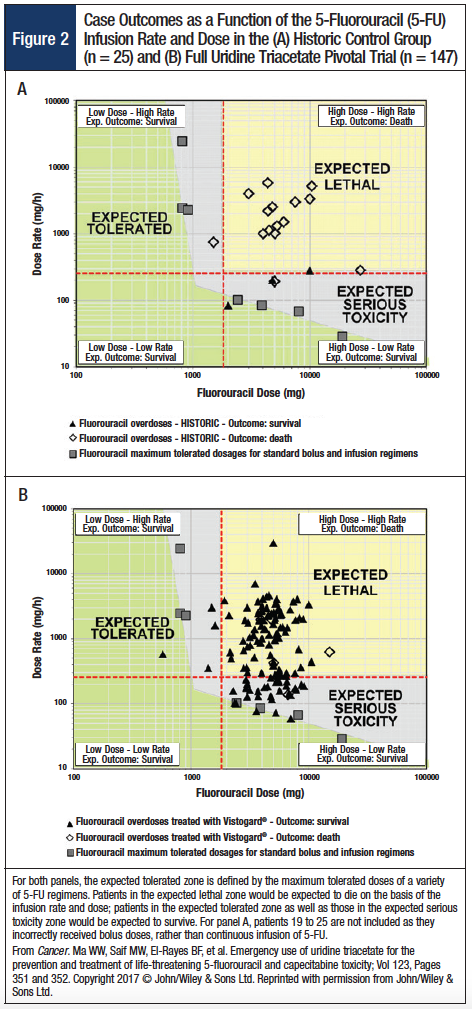
Preclinical studies had shown a 90% survival rate in mice when uridine triacetate was administered within 24 hours of a lethal dose of 5-FU.3 Furthermore, uridine triacetate was not genotoxic and was well tolerated in rats at a maximum feasible dose of 2000 mg/kg/day.3 Subsequent clinical trials,3,16 including part of the pivotal study data reviewed in this article, led to the FDA approval of uridine triacetate for the emergency treatment of patients with 5-FU or capecitabine overdose or early-onset severe or life-threatening toxicity within 96 hours of 5-FU or capecitabine exposure. Key to this approval was the clear survival benefit of uridine triacetate in the trial, which showed that 96% of patients receiving uridine triacetate survived compared with 16% of patients who received only supportive care in the historic cohort cited earlier.16 Notably, many patients who received uridine triacetate had 5-FU overdoses that would have likely been lethal in the supportive care cohort (Figure 2).16
As discussed previously, the timing of uridine triacetate administration was identified to be a crucial survival factor in the full evaluation of the pivotal study. For patients in the early-onset cohort, all 18 (100%) who initiated uridine triacetate treatment within 96 hours after the termination of 5-FU or capecitabine survived and recovered versus 3 of 8 (38%) who initiated treatment after 96 hours.16 All 6 adult patients (100%) in this study who had suicidal overdoses of capecitabine (ingestion of up to 28,000 mg all at once) and all 3 children (100%) who accidentally ingested capecitabine survived with minimal toxicities after receiving uridine triacetate within 96 hours of ingestion.16 Finally, to further illustrate the importance of initiating uridine triacetate treatment as soon as possible after overexposure to 5-FU or capecitabine, of the 10 deaths that occurred among the 173 patients in these studies, 5 (50%) were the previously mentioned patients from the early-onset cohort who received uridine triacetate after 96 hours; the remaining 5 deaths were in overdose patients who received the antidote within 96 hours but who had either progression of their underlying cancer (n = 3), septic shock leading to respiratory failure (n = 1), or apparent tumor lysis syndrome (n = 1) during the 30-day follow-up period.16
Because the efficacy of uridine triacetate has been established for only the 96-hour window after exposure to 5-FU or capecitabine, it is important for healthcare providers, patients, and caregivers to remain vigilant to the possibility of severe early-onset toxicity, particularly during the initial course or courses of treatment. Although certain genetic variants may predispose patients to 5-FU and capecitabine toxicity (ie, DPD, TS, OPRT), the absence of such mutations do not guarantee that early onset-onset toxicity will not occur. For example, DPD mutations are found in ≤50% of severe 5-FU toxicity cases.16 Therefore, evaluation of these predictive biomarkers is not routinely performed prior to initiating fluoropyrimidine therapy. It should also be noted that uridine triacetate’s mechanism of action is independent of these pathways, and that all patients exhibiting severe early-onset toxicity should be considered candidates for treatment. Furthermore, because of the rapid progression of toxicity and the high likelihood for a fatal outcome, prompt administration of uridine triacetate takes precedence over evaluating for the underlying molecular or genetic cause of the toxicity.
In the full analysis of the pivotal trial, uridine triacetate was shown to be well tolerated in patients with severe early-onset toxicity to or overdose with 5-FU or capecitabine.16 Nearly all reported adverse reactions that were possibly related to uridine triacetate were mild-to-moderate GI events. Those occurring in ≥2% of patients included vomiting (8.1%), nausea (4.6%), and diarrhea (3.5%). It is worth noting that these adverse events are similar to those occurring during routine chemotherapy, and that many of the patients in the pivotal trial experienced mucositis or other GI distress before receiving emergency treatment.
Conclusion
In pivotal clinical trials, uridine triacetate has proven to be a highly efficacious and safe antidote for treating overexposure to 5-FU and capecitabine when administered within 96 hours of exposure. Healthcare professionals should carefully monitor patients for symptoms indicative of 5-FU and capecitabine overexposure, particularly during the initial courses of treatment, to deliver this lifesaving treatment to patients who need it.
Acknowledgment
Timothy Silverstein, PhD, contributed to the development of this article.
References
1. National Institutes of Health, Public Health Service, HHS. Public teleconference regarding licensing and collaborative research opportunities for: methods and compositions relating to detecting dihydropyrimidine dehydrogenase (DPD). Fed Regist. 2008;73:38233.
2. Froehlich TK, Amstutz U, Aebi S, et al. Clinical importance of risk variants in the dihydropyrimidine dehydrogenase gene for the prediction of early-onset fluoropyrimidine toxicity. Int J Cancer. 2014;3:730-739.
3. Ison G, Beaver JA, McGuinn WD Jr, et al. FDA approval: uridine triacetate for the treatment of patients following fluorouracil or capecitabine overdose or exhibiting early-onset severe toxicities following administration of these drugs. Clin Cancer Res. 2016;22:4545-4549.
4. Becker K, Erckenbrecht JF, Häussinger D, Frieling T. Cardiotoxicity of the antiproliferative compound fluorouracil. Drugs. 1999;57:475-484.
5. Walko CM, Lindley C. Capecitabine: a review. Clin Ther. 2005;27:23-44.
6. Polk A, Vaage-Nilsen M, Vistisen K, Nielsen DL. Cardiotoxicity in cancer patients treated with 5-fluorouracil or capecitabine: a systematic review of incidence, manifestations and predisposing factors. Cancer Treat Rev. 2013;39:974-984.
7. Sternberg CN, Reichardt P, Holland M. Development of and clinical experience with capecitabine (Xeloda®) in the treatment of solid tumours. Eur J Oncol Nurs. 2004;8(suppl 1):S4-S15.
8. Xeloda® (capecitabine) tablets, for oral use [prescribing information]. South San Francisco, CA: Genentech USA, Inc; December 2016.
9. Hennessy BT, Gauthier AM, Michaud LB, Hortobagyi G, Valero V. Lower dose capecitabine has a more favorable therapeutic index in metastatic breast cancer: retrospective analysis of patients treated at M. D. Anderson Cancer Center and a review of capecitabine toxicity in the literature. Ann Oncol. 2005;16:1289-1296.
10. Longley DB, Harkin DP, Johnston PG. 5-Fluorouracil: mechanisms of action and clinical strategies. Nat Rev Cancer. 2003;3:330-338.
11. Schwab M, Zanger UM, Marx C, et al. Role of genetic and nongenetic factors for fluorouracil treatment-related severe toxicity: a prospective clinical trial by the German 5-FU Toxicity Study Group. J Clin Oncol. 2008;26:2131-2138.
12. Ichikawa W, Takahashi T, Suto K, Sasaki Y, Hirayama R. Orotate phosphoribosyltransferase gene polymorphism predicts toxicity in patients treated with bolus 5-fluorouracil regimen. Clin Cancer Res. 2006;12:3928-3934.
13. Kelsen DP, Martin D, O’Neil J, et al. Phase I trial of PN401, an oral prodrug of uridine, to prevent toxicity from fluorouracil in patients with advanced cancer. J Clin Oncol. 1997;15:1511-1517.
14. Bamat M, Tremmel R, Helton J, Von Borstel R. Clinical experience with uridine triacetate for 5-fluorouracil overexposure: an update. Ann Oncol. 2013;24(suppl 4). Poster P-0127.
15. Meulendijks D, van Hasselt JG, Huitema AD, et al. Renal function, body surface area, and age are associated with risk of early-onset fluoropyrimidine-associated toxicity in patients treated with capecitabine-based anticancer regimens in daily clinical care. Eur J Cancer. 2016;54:120-130.
16. Ma WW, Saif MW, El-Rayes BF, et al. Emergency use of uridine triacetate for the prevention and treatment of life-threatening 5-fluorouracil and capecitabine toxicity. Cancer. 2017;123:345-356.
17. Vaudo CE, Gil B, Galuski K, Zarwan C, Nugent FW. Early-onset 5-fluorouracil toxicity in a patient negative for dihydropyrimidine dehydrogenase mutations: the clinical course of reversal with uridine triacetate. Pharmacotherapy. 2016;36:e178-e182.
18. Saif MW, Von Borstel R. 5-Fluorouracil dose escalation enabled with PN401 (triacetyluridine): toxicity reduction and increased antitumor activity in mice. Cancer Chemother Pharmacol. 2006;58:136-142.
19. Fang L, Xin W, Ding H, et al. Pharmacokinetically guided algorithm of 5-fluorouracil dosing, a reliable strategy of precision chemotherapy for solid tumors: a meta-analysis. Sci Rep. 2016;6:25913.
20. Andreica IW, Pfeifer E, Rozov M, Tavares E, Shakurova A. Fluorouracil overdose: clinical manifestations and comprehensive management during and after hospitalization. J Hematol Oncol Pharm. 2015;5:43-47.
21. Accidental overdoses involving fluorouracil infusions. Institute for Safe Medication Practices (ISMP) website. www.ismp.org/newsletters/acutecare/showarticle.aspx?id=111. Published June 18, 2015. Accessed July 28, 2017.
22. Santos C, Morgan BW, Geller RJ. The successful treatment of 5-fluorouracil (5-FU) overdose in a patient with malignancy and HIV/AIDS with uridine triacetate. Am J Emerg Med. 2017;35:802.e7-802.e8.
23. Vistogard® (uridine triacetate) oral granules [prescribing information]. Gaithersburg, MD: Wellstat Therapeutics Corporation; December 2015.
24. Ashour OM, Naguib FN, el Kouni MH. 5-(m-Benzyloxybenzyl)barbituric acid acyclonucleoside, a uridine phosphorylase inhibitor, and 2',3',5'-tri-O-acetyluridine, a prodrug of uridine, as modulators of plasma uridine concentration: implications for chemotherapy. Biochem Pharmacol. 1996;51:1601-1611.